Your 3 Minute Knee Pain Assessment Latest
Engage in this 3 minute interactive experience to find out what evidence-based treatment is next for your knee pain.
The correct next step depends on your history, physical examination, and imaging. While we can’t give you medical advice, answer ALL questions and scroll to the END for an online recommendation, and a report you can discuss with your doctor.
To begin, which knee hurts?
Most people with knee pain have a strain, arthritis, a torn meniscus or torn anterior cruciate ligament.
Which one is causing your left knee pain? Study these pictures to find out.
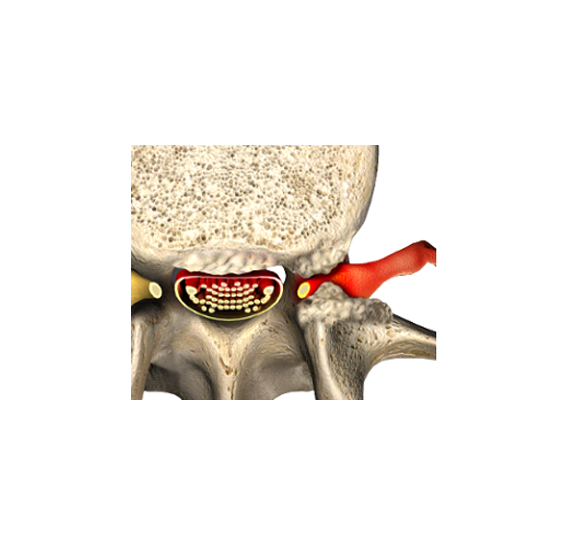
The knee joint consists of your kneecap in front, and the thigh and shin bones behind. The bones are separated by two meniscuses and held together by the anterior cruciate ligament (ACL).
The job of your meniscus is to cushion (absorbs) shock in the knee and prevent the thigh bone from touching and grinding against the shin bone during bending.
Each meniscus is a horseshoe shaped piece of cartilage.
A torn meniscus causes clicking, popping, and locking of the knee.
Click all that apply. My knee:
Because the meniscus is made of cartilage, and cartilage does not show up on x-ray, a torn meniscus does not show up on x-ray. That means you could have a normal x-ray and still have a badly torn meniscus.
You can suspect a torn meniscus by doing McMurray’s test on physical exam. In McMurray’s test an examiner bends and extends your knee with the shin bone rotated inward and outward. If the movement hurts and makes abnormal sounds, then McMurray’s test is positive.
My McMurray’s test IS:
If you don’t know, you can try McMurray’s test at home.
You need someone to help.
Since your left knee hurts, your helper should stand on your left.
Lay on your back. Have your helper bend your knee toward your chest, then rotate your shin bone inward while they straighten the knee. Repeat a few times. If there is clicking, popping, or pain while your knee moves then mark McMurray’s test positive above.
Repeat these steps but have the helper rotate your shin bone outward.
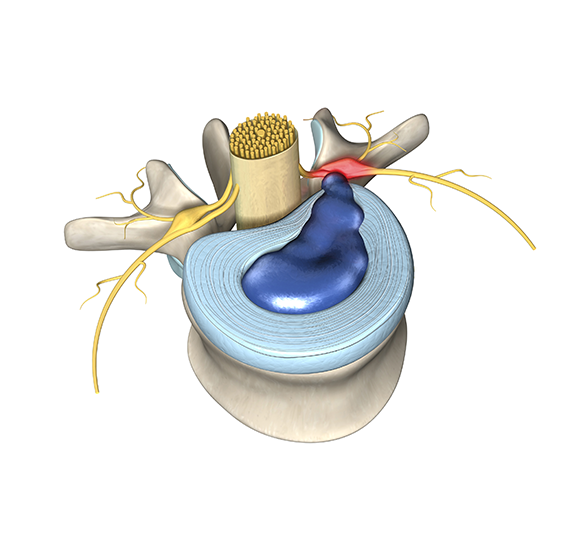
The thick, strong anterior cruciate ligament (ACL) connects and stabilizes the thigh bone to the shin.
A tear in the ACL makes the knee feel unstable, like it will give out when you walk.
Because the ACL is made of soft tissue, and soft tissue does not show up on x-ray, a torn ACL will not show up on x-ray. Just as in the case of a torn meniscus, your x-ray may be perfectly normal despite having severe knee pain and a torn ACL.
Your doctor may suspect an ACL tear by performing Lachman’s test on examination. In the Lachman test the examiner bends your knee to 30 degrees, then pressures the shin bone forward and the thigh bone back.
My Lachman’s test IS:
Again, if you don’t know, you can try Lachman’s test at home.You need someone to help.
Your helper should stand on the same side as the pain, like they did in the McMurray test. Your helper should bend your knee halfway toward your chest, place one hand behind your calf and the other on your thigh, and gently press your calf forward, and your thigh back. If the knee joint feels lax, or the painful side moves more than the normal one, then mark Lackman test is positive above.
Repeat these steps on the other knee for reference.
Note that in the first few weeks after an injury there will be too much muscle spasm and guarding to allow this test to be valid.
Your doctor will want to know when your pain started. This is triggering the video that is for the firs 3 weeks only. Don’t trigger the video.
And whether your pain is the result of an accident or injury. Did your knee pain begin with an accident or injury?
We are preparing a summary for you to share with your doctor or to use in finding a new one. Here’s what we have so far:
Do you mind if we ask how old you are?
Since osteoarthritis results from wearing down the cartilage in your knee it gets worse as you get older. Osteoarthritis is more common in women than men, but both get it.
Osteoarthritis is more common in people over 55, but it can happen at any age, and rarely even occurs in children.
The risk of arthritis is also increased in women, and with higher Body Metabolic Index.
Are you:
What is your BMI? Let’s see. Enter your weight and height:
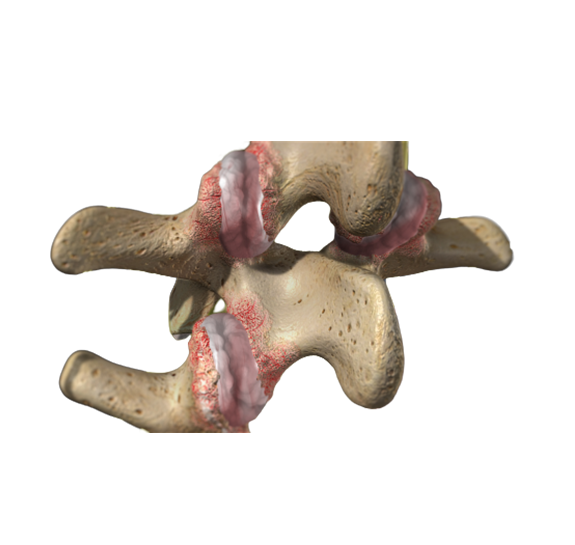
You have now seen what meniscus and anterior cruciate ligament (ACL) tears look like. The next thing we need to cover is the most common cause of knee pain: arthritis.
Arthritis causes thinning of the cartilage in the joint, rough surfaces, and can even result in loose bodies of cartilage floating in the fluid of the knee joint.
As it turns out, if you have severe arthritis your only effective treatment is knee replacement whether you have a meniscus or ACL tear or not. A knee x-ray is to find out if you have severe arthritis. So, even if you end up needing an MRI, it makes sense to get an x-ray to stage arthritis first.
Arthritis can be caused by an injury (post-traumatic), gradual degeneration of the smooth cartilage in the knee joint (osteoarthritis), or an inflammatory condition (rheumatoid or psoriatic).
Do you have arthritis?
Just FYI we continue to build the report for your doctor based on your responses.
Before we go on, we need to know if your knee problem is serious.
Your knee problem is serious if a delay in having MRI could cause further damage to your knee.
Red flags for knee pain:
- Associated fever, shakes, or chills
- Unexplained weight loss
- Cancer history
- Severe pain that prevents you from walking

Please Check any of these Red Flags that apply to you:
Have you done any of these already? Check all that you have done:
Here’s the rest of your summary so far:
Congratulations, you have almost made it to the end! We are preparing the report for your doctor, as well.
The last thing you need to know if you need an MRI of your left knee is the grade of arthritis on x-ray.
Have you had a recent x-ray of your knee?
Press this button to get your recommendation:
According to the information we have, your Summary Report looks like this:
Since you have not had an x-ray, your best next step is to get an x-ray. This will help determine if you need to follow-up with an MRI.
Your condition is complicated and requires hands-on care by a physician. Take the summary we have prepared for your doctor to discuss.
Sorry, we didn’t get to know you better. Some people learn better by taking a course. Click here for our “Do I need an MRI of my knee?” course.