MINIMALLY INVASIVE SPINAL FUSION
“Surgery” is the last word you want to hear when you’re looking for treatments for back pain. But, if your pain has lasted longer than 12 weeks, surgery is the may be the best option. In the first 12 weeks, your doctors will try noninvasive treatments for your back pain, but there are some conditions that noninvasive methods cannot treat.
Spinal fusion is a frequently performed type of back surgery. This procedure can help reduce pain and relieve the symptoms of many back conditions.
WHAT IS SPINAL FUSION?
As the name suggests, spinal fusion is the process of connecting two or more joints in the spine. This causes these vertebrae to lose mobility, which provides better support and stability in the spine, and helps reduce pressure on the nerves passing through your spine.
Surgeons complete a spinal fusion procedure in two steps:
- Removes the cartilage and other soft tissues from the disc and/or facet joint and roughen up the bony surfaces.
- Hardware will be placed in the spine that limits its movement.
Limiting the movement of your vertebrae is what allows the fusion to take place. Your body will recognize the roughened bony surfaces as a fracture, and sets forth on building new bone tissue to heal. As this takes place, the separate bones that are held together by hardware will fuse together into one solid piece.
WHAT DOES SPINAL FUSION TREAT?
The main objectives of spinal fusion are to improve your stability and reduce pain. Studies have shown it is a reliable treatment method for many conditions. Spinal fusion is always the last resort to noninvasive methods, but many conditions can’t get better without it:
- Spinal fractures causing instability
- Painful, torn discs
- Spinal deformities, such as scoliosis
- Spondylolisthesis
- Tumors and bone infections causing instability
Spinal fusion can take place anywhere along the spine where it is the best treatment option for pain. Traditionally, there are three areas of the spine that undergo spinal fusion:
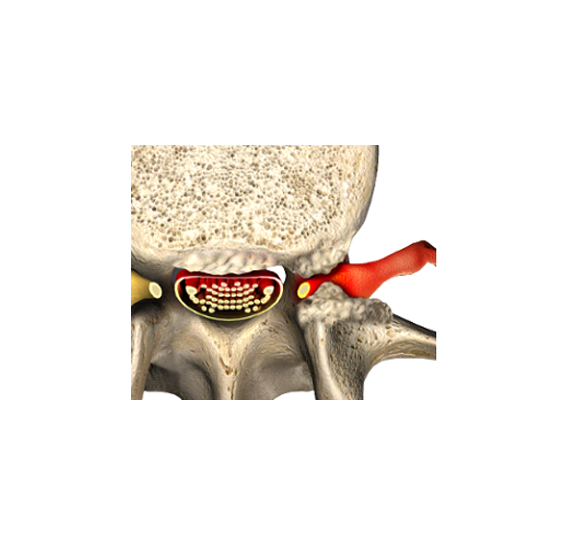
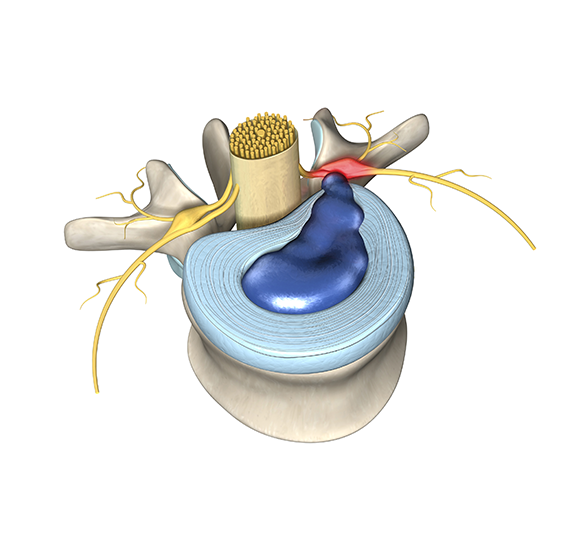
- Fusion between vertebrae after the removal of a disc — The soft discs that usually cushion the vertebrae may need to be removed if they are torn and causing pain.
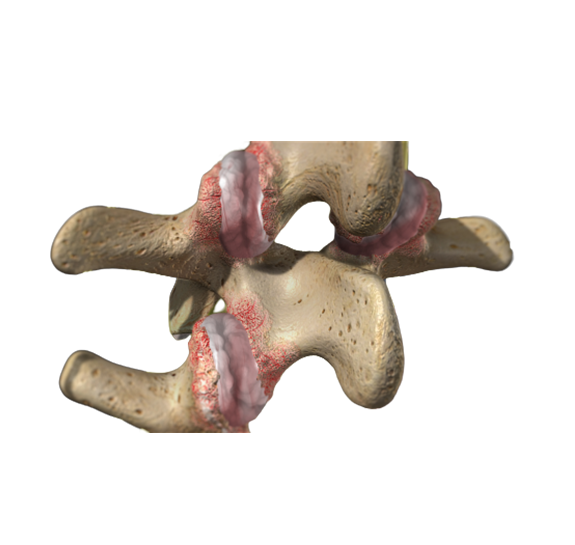
- Fusion of the facet joint — Fusion can help support the spine when a facet joint is damaged by conditions that wear down its cartilage.
- Fusion of the transverse processes of the vertebrae — This type of fusion is rarely done anymore because there are more effective, less-invasive options.
WHAT ARE THE BENEFITS OF SPINAL FUSION?
Spinal fusion can be intimidating because it limits the mobility of your vertebrae. However, most fusions affect a small part of your spine, so many spinal fusion patients do not notice much of a difference in their mobility. The limitation of mobility itself isn’t exactly a benefit of the procedure, but it’s good to know it may not be as big of an issue as you think.
Benefits of spinal fusion surgery include:
- Improved mobility — Although mobility is limited at the site of the fusion, the reduction of pain may actually allow you to regain more complete use of the rest of your spine.
- Less pain
- Better alignment of the spine, which reduces the wear and tear misalignment can create
- Long-term solution to back pain and injuries
- Most patients can go home the same day of the surgery
- Living a life free of medications and their side effects
ARE THERE RISKS IN SPINAL FUSION?
Spinal fusion surgery comes with some risks that are worth considering before undergoing the procedure. These risks may include:
- Infection
- Pseudoarthrosis — This is a condition that limits the bone formation after your surgery. People who smoke have a high chance of developing this condition.
- Loss of blood
- Leaking spinal fluid
- Nerve damage
- Pain in the graft site — Some doctors use bone grafts taken from your pelvis. This can cause long term pain at the donor site.
HOW LONG DOES IT TAKE TO RECOVER FROM SPINAL FUSION?
Spinal fusion surgery is usually a quick procedure that is finished within a couple of hours. Patients need some time to recover from anesthesia afterward but are generally able to go home on the same day of the procedure.
Each patient is different, so your post-operative instructions may vary. You will usually be asked to take a 10-minute walk each day for a week after surgery, 20-minute walks during the second week and 30-minute walks during the third. At that point, we ask you to begin exercises to strengthen your core.
Pay attention for signs of infection after your procedure. Your doctor will need to address these immediately to identify and treat any infection. Symptoms of infection include:
- Drainage from the incision
- Redness and swelling around the incision
- A fever over 100 degrees
- Chills